Is the social impact workforce ready for the next emergency?
Reimagining capacity: Building the workforce for future preparedness
Why It Matters
COVID-19 exacerbated many deadly health emergencies — including the opioid crisis — and limited the social impact sector’s ability to respond. Lessons from this time can help build readiness to respond to all types of catastrophes more effectively and proactively.
This story is in partnership with the Canadian Red Cross.
“I know what it’s like to be looked at as the bottom-of-the-barrel of society. I remember standing in line at the methadone clinic and people writing me off as a human being just because of where I was,” says Chris Cull, now nine years into his recovery from an opioid addiction.
Today, Cull is a lived experience advocate who volunteers his time helping organizations and governments improve the prevention and treatment of substance misuse. Cull says his lived experience makes his advocacy and volunteerism even more crucial. And he says the need is greater today, still in the throes of the COVID-19 pandemic, which exacerbated Canada’s opioid crisis.
“It’s always getting worse,” says Cull. “There’s never been a time in my 15 years where I’ve seen it getting better. The problem is that it’s always evolving quicker than we are.”
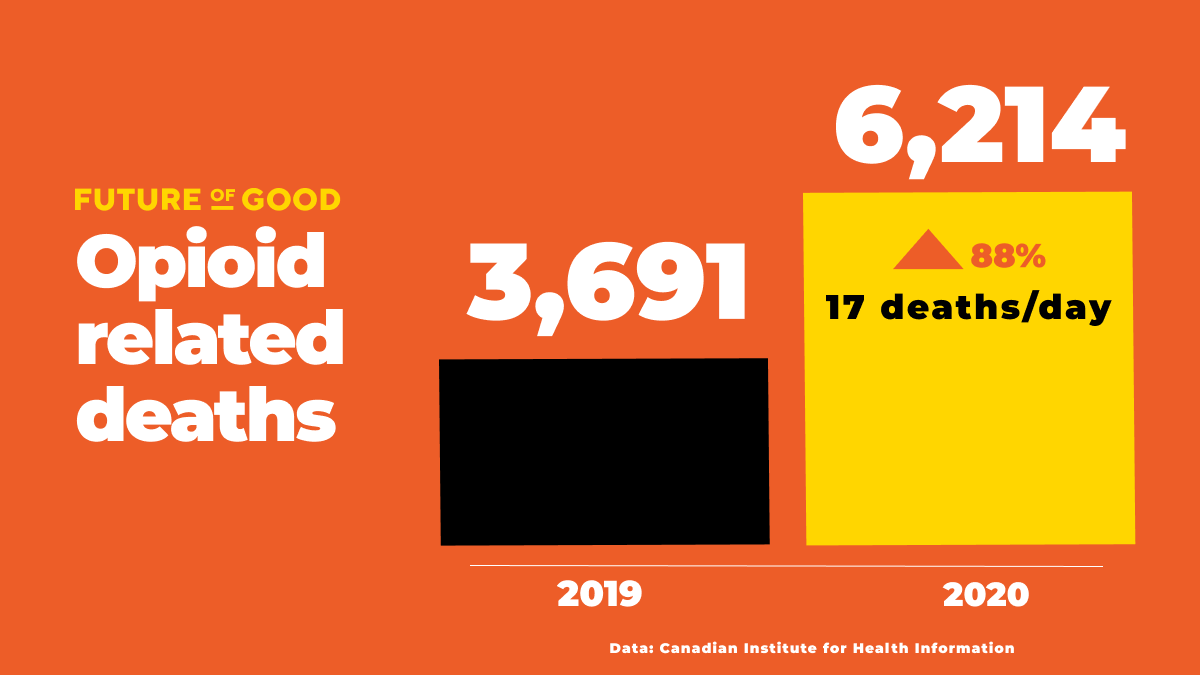
Since the onset of the pandemic, 6,946 opioid-related deaths occurred (between April 2020 to March 2021), which is an 88 percent increase from the same time period prior to the pandemic (April 2019 to March 2020 – 3,691 deaths, all based on data from the Canadian Institute for Health Information). All told, in 2020, opioid misuse was responsible for approximately 17 deaths a day in this country (a total of 6,214 deaths overall), and nearly all of those deaths (96 percent) were accidental. The rise in deaths is due at least in part, experts say, to people experiencing heightened feelings of isolation, stress and anxiety, and limited availability or accessibility of services for people who use drugs.
Some have dubbed the opioid crisis one of many ‘shadow pandemics’ — like gender-based violence, homelessness, growing levels of economic inequality and declining mental health — an existing public health crisis obscured by another one, the pandemic, but having reached a boiling point.
Hidden behind the figures are the mental health and substance use workforce, an already fragmented and undervalued workforce pre-pandemic, now pushed to their limits. Mobilizing this workforce to address the opioid crisis offers crucial learning for future emergency response and preparedness — primarily, to build a more resilient frontline, requires supporting and investing in the workforce.
Workforce grief and trauma
Rebecca Jesseman is the director of policy at the Canadian Centre on Substance Use and Addiction, a national non-profit with a mandate to reduce the harms associated with substance use in Canada. Jesseman worries about what’s behind the “staggering” opioid-related figures, for example, misuse and overdose that led to harm, but not death. And that raises another concern — the toll on first responders due to pandemic-related burnout, trauma, and grief, compounded by the trauma they already experience given the nature of their day-to-day work.
“What do the significant long-term health and emotional impacts mean for the people who are responding?” asks Jesseman. “If you think of people responding in this crisis-situation, what does that do to your emotional regulation and always being in that crisis-response-mode? What are the long-term impacts on the service providers?”
One U.S. study estimated that for every death from COVID-19, on average, nine people are left in grief. Healthcare workers like Gelsa de Oliveira, a nurse deployed with the Canadian Red Cross in COVID-19 intensive care units in Toronto-area hospitals, says nurses and other healthcare providers are often the ones spending the final minutes with patients dying from COVID-19.
“It’s very stressful, it’s overwhelming. It can cause a lot of trauma in the nurses. We’re there to save lives but there wasn’t a lot we could do. It’s like you’ve been at war. You try to protect yourself, protect your family, protect your patients, protect your coworkers but it’s sometimes out of control,” says de Oliveira, who delayed her own retirement to help battle the pandemic, saying she felt compelled by the mission of the Canadian Red Cross to do whatever she could to alleviate the suffering on her patients and fellow providers.
But for those who work in the mental health and substance use sector, the loss of life by overdose this past year has compounded the grief and trauma they routinely experience as part of their routine work.
“Lots of burnout, lots of trauma, really hard work that people have been doing and were doing before the pandemic, and it just got that much harder during a pandemic,” says Dr. Mary Bartram of the pandemic experience for the mental health and substance use workforce across Canada. Bartram is director of policy at the Mental Health Commission of Canada, a national non-profit working to improve mental health services, supports and policies. She says this workforce often brings lived experience to their role, and with that experience often comes trauma, not to mention that which happens by nature of the job, often poorly supported and underrecognized. “This workforce makes a lot of room for the expertise that comes from lived experience, but the system doesn’t always provide enough support, remuneration, access to certification or regulation,” says Bartram.
The answer? To build a more resilient frontline, invest in the workforce
“The substance use workforce in Canada is largely unregulated. It’s underfunded,” says Jessemen.
She adds that an assessment of the workforce’s needs is step one. “We don’t have a good picture of what the substance use workforce looks like and where the significant gaps are because we just don’t have good data. A very preliminary step is improving our data collection so that we can better identify the gaps.”
Dr. Ivy Bourgeault, the Canada Research Chair in Comparative Health Labour Policy at the University of Ottawa, agrees: fulfilling pressing mental health and substance use needs, she says, requires a “whole-of-health-workforce approach” and only then can the effort be proactive versus reactive. “We need to get our house in order and know what exactly is in our house so that we can then say, ‘What is it that we need to support? Do we have enough of these workers? How are they trained? What additional training might they need in order to be more nimble?’”
Less than one percent of health research funds goes toward the health workforce, which is disproportionate considering the workforce makes up 70 percent of health system costs and 8 percent of Canada’s Gross Domestic Product, says Bourgeault. “It’s particularly problematic given this is a sector that’s highly gendered, female. From an international perspective, one of the most feminized health workforces is in Canada,” says Bourgeault.
Bartram says the Canadian Institute for Health Information offers “skeleton” information about some of the providers that are commonly thought of in the mental health workforce, but argues it’s high-level and doesn’t lend insights to substance use workers, whether the workforce is full-time or part-time, nearing retirement, and it does not offer insights into their level of training or well-being.
“None of the things that really help with planning, frankly” says Bartram, adding workforce information is necessary for coordinating health human resources in routine times, but especially to address emergent crises. “We need data to support effective planning, and without that, our efforts to be more proactive are going to continue to be severely restricted. It’s like having two hands tied behind your back to try to do planning in this sector.”
The pandemic has shown what’s possible in emergency response
As much as the added pressures of the pandemic brought despair, it has also supplied evidence that a swift response is possible in mobilizing the public health workforce. Dr. Andrew Boozary, a primary care physician and executive director of the University Health Network’s social medicine program in Toronto, says he would like to see that same attention brought to the other public health emergencies like the deadly opioid crisis.
“We’ve always been told it cannot be done or cannot be done quickly enough,” says Boozary. “We’ve done it at a pace that we’ve not seen before. And I think when you look at what the pandemic has taught us, hopefully there are a lot of lessons learned that we can actually leverage to improve public health.”
Among those key lessons, says Boozary, is how political will and urgency can break down barriers that once seemed insurmountable. One of the high points of seeing the pandemic response unfold, he says, is seeing multiple levels of government come together to sing from the same song sheet. This is in line with the federal government’s response, “Emergency Management Strategy for Canada: Toward a Resilient 2030, recognizing, “Resilient capacity is built through a process of empowering citizens, responders, organizations, communities, governments, systems and society to share the responsibility to keep hazards from becoming disasters.”
The Canadian Red Cross mobilized quickly to respond to COVID and its knock-on effects, too, largely through partnerships with local organizations that were already tapped into communities and their needs, says Cheryl Tompkins, the organization’s deputy director of community health services. For example, when lockdown first came into effect in Toronto in 2020, the Canadian Red Cross worked with both the City of Toronto and the Daily Bread Food Bank. All three organizations collaborated on a food delivery program and a call centre to help clients figure out whether they were eligible for the program.
“Partnerships are often successful when there is a history of working together to serve the same geography and demographic,” Tompkins says. “Together, we share our knowledge of the environment and identify the gaps and available resources when responding to communities.
That’s also in keeping with lessons learned from countries that led the most successful pandemic responses. According to The Independent Panel for Pandemic Preparedness and Response, which tabled its report in May this year, countries leading a successful response (with “success” measured as keeping disease transmission and deaths as low as possible) coordinated their country-level efforts by establishing partnerships across sectors, including community leaders, and levels of government, as well as the private sector. “Where community structures, such as cadres of community health workers, have been mobilized, they have made a critical difference in establishing trust in government instructions, extending services, and in relaying scientific information,” found the panel. Countries that were able to manage surge health workforce demands did so through “mobilizing, training and reallocating their health workforce with a combination of hiring new staff, using volunteers and medical trainees and mobilizing retirees.”
In the case of the Canadian Red Cross partnerships with the City of Toronto and the Daily Bread Food Bank, Tompkins said they found a wealth of capable and knowledgeable response workers. “Staff and volunteers from across multiple programs, including health and emergency management and from other geographies were seconded to support the program,” Tompkins says.
In contrast, the panel found “The health systems which had been under-resourced and fragmented over a long period prior to the pandemic were the least resilient.”
Back in Bowmanville, Ontario, Chris Cull’s motivation to keep pressing for better mental health and substance use support comes from a place of lived experience, knowing what it’s like to be left isolated and disconnected from services.
“I’m a big believer that we’re at least as strong as society’s most vulnerable,” says Cull, who wants to see more attention paid to ramping up Canada’s workforce and capacity for getting urgent mental health and substance use care to those at the frontline of the opioid crisis.
That includes recognizing volunteers, who have continued to offer their time both formally through charities, non-profits, and community organizations and informally providing essential services: “They are providing shelter and services to the homeless, and to women and children fleeing violence; help for isolated seniors; mental health services for children; ongoing and emergency food and other provisions within communities,” finds a new report released by Statistics Canada on volunteerism in Canada. In 2018 (the most recent year for which this information is available), almost 12.7 million people volunteered for charities, non-profits and community organizations — that’s 41 percent of Canadians aged 15 and older and the equivalent of more than 863,000 year-round full-time equivalents (FTEs). Add to that the nearly 22.7 million people who volunteered informally — accounting for 74 percent of Canadians aged 15 and older and 1.8 million FTEs
Cull says the ways to address the opioid crisis are there, but creating the will requires addressing the pervasive stigma those with addictions face. “Addressing the stigma is foundational to any solution,” agrees Jesseman, “That’s what we need to do to open the door to having reasonable conversations.”
A Canada-wide emergency response strategy
And on an even more long-term scale, Canada’s various levels of government should partner with civil society organizations to build a country-wide preparedness plan for future emergencies like COVID-19 and the cascading opioid crisis — centring a well-equipped and ready workforce, says Stephane Michaud, vice president of internal operations at the Canadian Red Cross. Having a network of people ready to respond to communities’ needs in a matter of days — not weeks or months — would alleviate some of the pressure on existing workforces, and better serve communities themselves.
“One way to achieve this goal is to broaden the scope of possibilities through a network of interlinked local and global responses, allowing experts to respond and assist in each other’s emergencies, honing their skills through exposure to events they would otherwise never see in their own geography, while respecting the primacy of local interventions,” Michaud says. “For example, the Canadian Red Cross has been working side by side with partners facing outbreaks of Ebola, Zika, cholera and measles for years and that allowed us to rapidly pivot and provide a vast array of support to the COVID-19 pandemic response in Canada. We could do that because we had recent and relevant experience that could not have been acquired on the scale of a single country.”
Experts say emergencies are here to stay — especially climate disasters, which will become more frequent and severe in the coming years — and a coordinated, well-resourced response network could be what gets the country through it.
Should you need any support, please contact any of the following resources:
- Crisis Services Canada 1-833-456-4566
- Centre for Addiction and Mental Health 1-800-463-2338
- Wellness Together Canada (Adults: Text WELLNESS to 741741; Front Line Workers: Text FRONTLINE to 741741)
- Kids Help Phone 1-800-668-6868
- First Nations and Inuit Hope for Wellness Help Line 1-855-242-3310
- Trans LifeLine 1-877-330-6366
- Strongest Families Institute 1-866-470-7111
Your job. Your mission. Your news.
With your support, the sector you're building gets the journalism it deserves, and you get a tax receipt.



