Canada’s first COVID-19 vaccine is on the way. How can the social impact world make sure it gets to those who need it most?
Black residents of Canada’s largest city are only about 9 percent of the population, yet comprise 24 percent of Toronto’s COVID-19 cases
Why It Matters
Canada just approved a COVID-19 vaccine. Meanwhile, Toronto’s Black community is getting infected with COVID-19 at disproportionately high rates. Medical inequities and distrust are part of the problem and the incoming vaccine may not be enough.
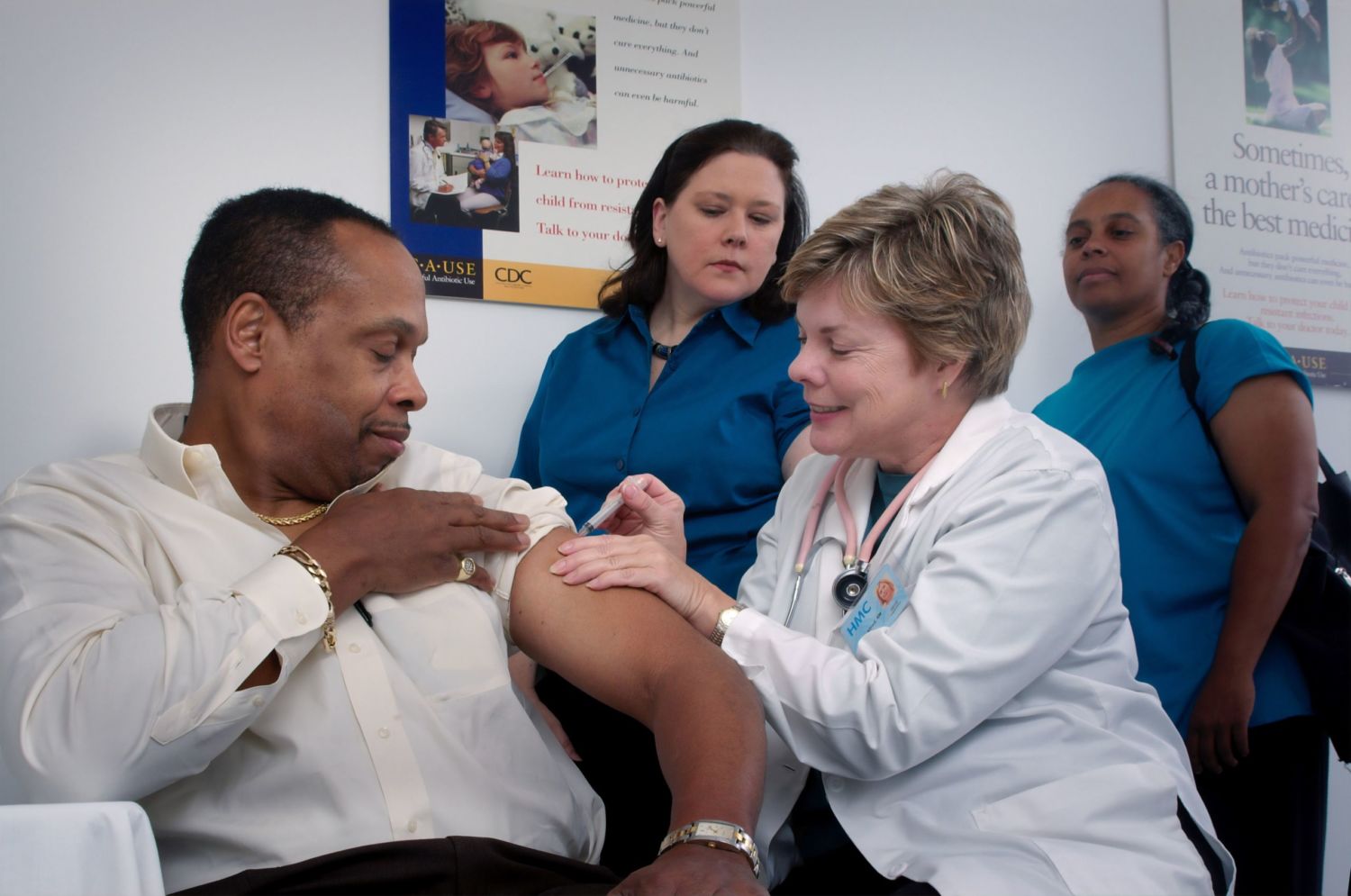
Canada has approved the Pfizer COVID-19 vaccine, and the first shipment of a quarter-million doses could arrive at distribution centres and clinics by the end of 2020, an unheard of record for vaccine deployment in modern medical history. Muhaari A., director of health promotion at Black Coalition for AIDS Prevention, doesn’t believe the vaccine will reach everyone in Toronto who requires it.
HIV/AIDS and COVID-19 are two completely different diseases. But their impact on Toronto, Canada’s largest and most diverse city, might be similar if the federal government isn’t careful. When the HIV/AIDS pandemic arrived in Toronto in the 1980s, it was also a highly complex and mysterious disease that largely affected the most marginalized members of society at the time — LGBTQ+ people and intravenous drug users among them. Later, infections among the Black and Caribbean communities rose, and the demographic is still among the more likely groups to be diagnosed with HIV/AIDS.
As of December, Black people make up 24 percent of Toronto’s confirmed COVID-19 cases despite only comprising about 9 percent of the population. Middle Eastern residents are also disproportionately likely to be infected than the city’s white population. Heat maps of Toronto infections show huge hotspots in the east Toronto region of Scarborough, as well as Black neighbourhoods in the city’s northwest. There is a good reason why. Many Black and racialized people don’t have the luxury of working from home. Some work in frontline roles, including the very hospitals and clinics tackling the outbreak. “We keep praising doctors and nurses. But who cleans up after them?” says Muhaari (who declined to give his last name). “They’re the custodians and the janitors. They’re the people who look like us. And a lot of them are not supported.”
Black people make up 24 percent of Toronto’s confirmed COVID-19 cases despite only comprising about 9 percent of the population.
The federal government has promised that every Canadian who wants a COVID-19 vaccine will be able to get one, according to an as-of-yet undetermined priority system. The government does cover the cost of HIV/AIDS medications now, Muhaari says – which can run $1600 or more every month. But for those who are undocumented or are do not have proper access to the medical system, this cost is prohibitive. Muhaari says the government’s approach to fighting HIV/AIDS does not bode well for how it will ensure a COVID-19 vaccine is equitably distributed among Black people in Canada’s largest city.
“I’m happy there is a vaccine, but I think Black folks will not see it soon,” he says in an interview just days before Canada’s approval of the Pfizer vaccine. “If we cannot even have full coverage for HIV medication, I would not lie to myself that we are getting the vaccine soon.” Distributing a COVID-19 vaccine in an equitable manner in Toronto (and across Canada) will require far more than a comprehensive logistical plan. It will mean consulting with racialized residents in Toronto on vaccine deployment, combating misinformation, and establishing the most valuable asset in public health — trust. And social impact organizations working in Toronto are already doing this work.
Systemic racism in the medical system is not new for Black people, in Toronto or elsewhere. Precise data on anti-Black racism in the Canadian medical system is lacking, but a recent investigation in B.C. found 84 percent of Indigenous patients in the province’s healthcare system experienced some form of discrimination. In the United States, numerous studies have shown the Black community has a distrust of the medical system — and vaccines in particular, thanks to historical atrocities like the Tuskegee experiment, a study where hundreds of Black men with untreated syphilis were given placebos without their knowledge to study the virus’s fatal progression.
When it comes to the Black, African, and Caribbean community in Toronto, establishing the legitimacy of a COVID-19 vaccine is critically important. “A lot of work has to be done to build trust and to say, this is actually for our own good,” says Ky’okusinga Kirunga, director of the African and Caribbean Council on HIV/AIDS in Ontario. “We need to own it. We have to protect ourselves, our community, our families. We need to get this vaccine.” One easy way to do that is getting community members involved in the decision-making processes around vaccine distribution at the very start, rather than running a consultation process as an afterthought.
There’s a role for social impact organizations to play in guiding equitable distribution and fighting misinformation about COVID-19 — not just the vaccine. 211 Central, a call service that connects people with social services in the Toronto area, began noticing an increasing reluctance to get tested and started notifying its partner agencies in the area. “That’s going to be tricky to deal with in terms of testing, but also important to think about when thinking about who gets the vaccine and when are these communities that are more deeply impacted,” says Carrie Moody, director of strategic services at 211 Central. “They’re living in closer quarters and they’re living in multi-generational housing. That’s definitely something that our partners are very concerned about.”
There’s a role for social impact organizations to play in guiding equitable distribution and fighting misinformation about COVID-19 — not just the vaccine.
Muhaari and Kirunga are also worried. Misinformation was rampant during the HIV/AIDS pandemic: that only gay men spread it, that Black people spread it, that the virus could be transmitted simply by sharing food. Decades later, some of these myths still persist, even with reams of medical evidence. With COVID-19, it is still quite difficult to answer some of the most basic questions about the virus, potential vaccines, and their distribution. “We don’t know much about the facts. I wish I could know more because people would start coming to us,” Muhaari says. “For us, we build trust by giving correct information on time, and countering the negative messages — on time.”
Then there are the logistical challenges. While a multitude of agencies, including the Canadian military, will help distribute COVID-19 vaccine doses across the country, there are some challenges Black and racialized communities in Toronto will face in receiving the two-dose Pfizer vaccine. For one, it must be kept at -70 C in a special ultra-low temperature freezer. Canada has purchased 26 of them, and only 9 have been produced as of December. “No community health centre will have that,” Muhaari says.
Getting the vaccine will also pose trouble for anyone who must travel a long way to access medical care, as is often the case in Toronto neighbourhoods such as Scarborough and the city’s northwest that are both very diverse and have great healthcare needs. “I have patients who don’t follow up as often as I would like them to because of travel,” Dr. Avnish Mehta, a community health centre doctor, told The Local in 2019. “I think that’s pretty universal within Scarborough.” What if getting a two-dose vaccine requires travelling for hours from Scarborough to a health centre downtown? “That alone might prevent me from getting access,” Muhaari says. For someone who is undocumented or doesn’t have a health card, travelling to receive a vaccination may not be an option at all. While many of Toronto’s public services are available in commonly spoken languages such as Hindi, Urdu, and Arabic, accessing a vaccine could be difficult for someone who cannot use their preferred language to do so.
And then there are the issues posed by Pfizer’s vaccine. It is a two-step process, requiring shots a month apart. “You lose a lot of people that way,” Kirunga says. Someone who is homeless may not be able to follow up for the second shot. So, too, might someone working multiple jobs across different cities with an unpredictable schedule. This may only be an issue with Pfizer — the remaining six vaccine candidates purchased by Canada are single-shot. Still, this issue shows just how intertwined a vaccine’s deployment is with issues of social justice, access, and medical equity.
Many of these problems are complex issues that the Canadian social impact sector may not be able to tackle on its own — but can guide with expertise and evidence. Producing and distributing the vaccine is, of course, the responsibility of federal and provincial governments. Much of the information around COVID-19 is coming from public health units. Determining who is eligible for the vaccine — and when they might receive one — will be the responsibility of numerous agencies, departments, and ministries, but social impact organizations could provide the community knowledge to guide an equitable rollout.
The sector is also well-equipped to tackle misinformation and stay in close communication with the most marginalized communities as more information on the vaccine’s rollout becomes available. Its insights may even be of use to governments planning the vaccine deployment. “If you are listening to community workers who are out there or outreach workers…that would tell you a lot more about what is going on out in the community, and I think that would be very helpful in assisting a plan,” Muhaari says.
Organizations such as Black CAP and the African and Caribbean Council on HIV/AIDS in Ontario have spent years fighting stigma and providing clear and consistent information on a deadly virus to communities that often see systemic racism at the hands of the medical system. The lessons they’ve learned about combating misinformation and considering equitable medical access are also very applicable to the COVID-19 pandemic — and other social impact organizations looking to take part in an equitable vaccine deployment.
Even if the vaccination deployment is a resounding success, there will still be plenty of work to do, as there still is with HIV/AIDS and so many other deadly diseases in Canada right now. Rich and poor neighbourhoods across Toronto will continue to see COVID-19 cases after the vaccine is deployed. The differences will lie in how easily their residents will be able to access treatment and schedule a vaccination. “People think that once the vaccine is available, COVID will end,” Muhaari says. “No, it won’t. There will still be cases going on.”



